
Face Masks: What the Spanish Flu Can Teach Us About Making Them Compulsory
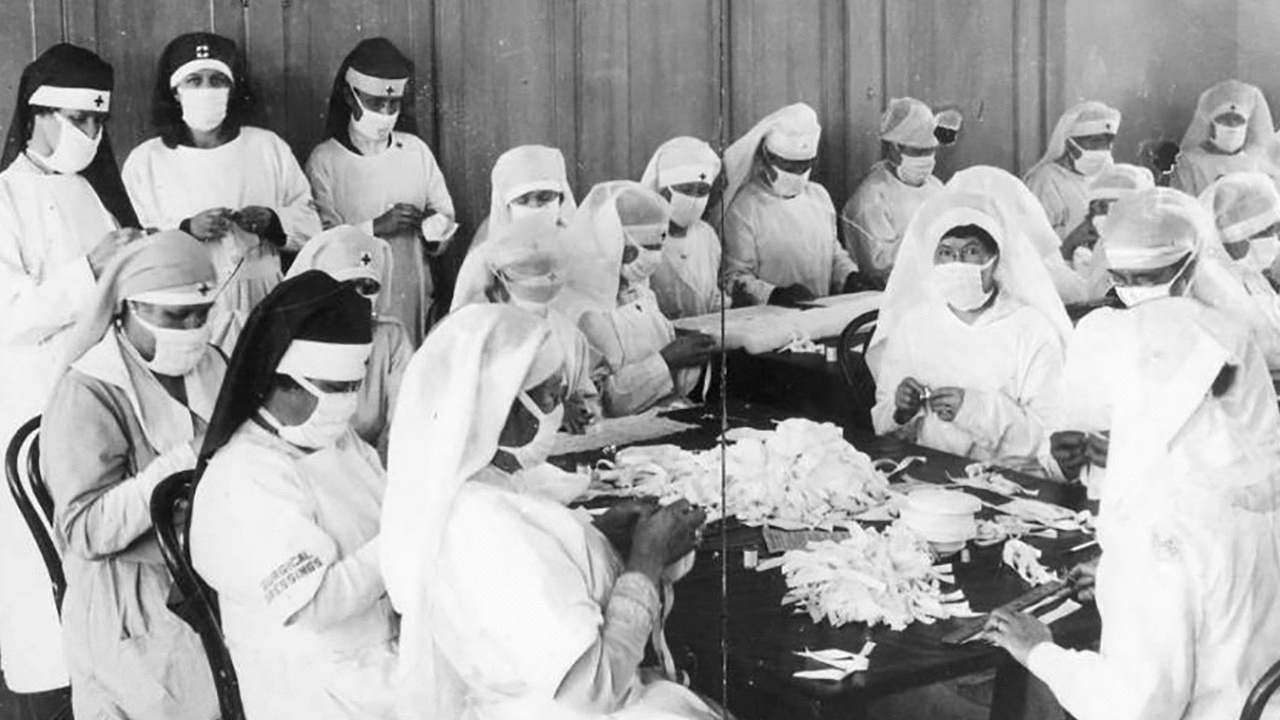
Red Cross nurses in San Francisco, 1918. Wikimedia
By Samuel Cohn
Should people be forced to wear face masks in public? That’s the question facing governments as more countries unwind their lockdowns. More than 30 countries have made masks compulsory in public, including Germany, Austria and Poland. This is despite the science saying masks do little to protect wearers, and only might prevent them from infecting other people.
Nicola Sturgeon, the Scottish first minister, has nonetheless announced new guidelines advising Scots to wear masks for shopping or on public transport, while the UK government is expected to announce a new stance shortly. Meanwhile, U.S. Vice President Mike Pence has controversially refused to mask up.
This all has echoes of the great influenza pandemic, aka the Spanish flu, which killed some 50 million people in 1918-20. It’s a great case study in how people will put up with very tough restrictions, so long as they think they have merit.
The Great Shutdown
In the U.S., no disease in history led to such intrusive restrictions as the great influenza. These included closures of schools, churches, soda fountains, theatres, movie houses, department stores and barber shops, and regulations on how much space should be allocated to people in indoor public places.
There were fines against coughing, sneezing, spitting, kissing and even talking outdoors — those the Boston Globe called “big talkers.” Special influenza police were hired to round up children playing on street corners and occasionally even in their own backyards.
Restrictions were similarly tough in Canada, Australia and South Africa, though much less so in the UK and continental Europe. Where there were such restrictions, the public accepted it all with few objections. Unlike the long history of cholera, especially in Europe, or the plague in the Indian subcontinent from 1896 to around 1902, no mass violence erupted and blame was rare — even against Spaniards or minorities.
Face masks came closest to being the measure that people most objected to, even though masks were often popular at first. The Oklahoma City Times in October 1918 described an “army of young women war workers” appearing “on crowded street cars and at their desks with their faces muffled in gauze shields.” From the same month, The Ogden Standard reported that “masks are the vogue,” while the Washington Times told of how they were becoming “general” in Detroit.
Shifting Science
There was scientific debate from the beginning about whether the masks were effective, but the game began to change after French bacteriologist Charles Nicolle discovered in October 1918 that the influenza was much smaller than any other known bacterium.
The news spread rapidly, even in small-town American newspapers. Cartoons were published that read, “like using barbed wire fences to shut out flies.” Yet this was just at the point that mortality rates were ramping up in the western states of the U.S. and Canada. Despite Nicolle’s discovery, various authorities began making masks compulsory. San Francisco was the first major U.S. city to do so in October 1918, continuing on and off over a three-month period.
Alberta in Canada did likewise, and New South Wales, Australia, followed suit when the disease arrived in January 1919 (the state basing its decision on scientific evidence older than Charles Nicolle’s findings). The only American state to make masks mandatory was (briefly) California, while on the east coast and in other countries including the UK they were merely recommended for most people.

San Francisco gathering, 1918. Wikimedia
Numerous photographs, like the one above, survive of large crowds wearing masks in the months after Nicolle’s discovery. But many had begun to distrust masks, and saw them as a violation of civil liberties. According to a November 1918 front page report from Utah’s Garland City Globe:
The average man wore the mask slung to the back of his neck until he came in sight of a policeman, and most people had holes cut into them to stick their cigars and cigarettes through.
Disobedience Aplenty
San Francisco saw the creation of the anti-mask league, as well as protests and civil disobedience. People refused to wear masks in public or flaunted wearing them improperly. Some went to prison for not wearing them or refusing to pay fines.
In Tucson, Arizona, a banker insisted on going to jail instead of paying his fine for not masking up. In other western states, judges regularly refused to wear them in courtrooms. In Alberta, “scores” were fined in police courts for not wearing masks. In New South Wales, reports of violations flooded newspapers immediately after masks were made compulsory. Not even stretcher bearers carrying influenza victims followed the rules.
England was different. Masks were only advised as a precautionary measure in large cities, and then only for certain groups, such as influenza nurses in Manchester and Liverpool. Serious questions about efficacy only arose in March 1919, and only within the scientific community. Most British scientists now united against them, with the Lancet calling masks a “dubious remedy.”
These arguments were steadily being bolstered by statistics from the US. The head of California’s state board of health had presented late 1918 findings from San Francisco’s best run hospital showing that 78 percent of nurses became infected despite their careful wearing of masks.
Physicians and health authorities also presented statistics comparing San Francisco’s mortality rates with nearby San Mateo, Los Angeles and Chicago, none of which had made masks compulsory. Their mortality rates were either “no worse” or less. By the end of the pandemic in 1919, most scientists and health commissions had come to a consensus not unlike ours about the benefits of wearing masks.
Clearly, many of these details are relevant today. It’s telling that a frivolous requirement became such an issue while more severe rules banned things like talking on street corners, kissing your fiancé or attending religious services — even in the heart of America’s Bible belt.
Perhaps there’s something about masks and human impulses that has yet to be studied properly. If mass resistance to the mask should arise in the months to come, it will be interesting to see if new research will produce any useful findings on phobias about covering the face.
Reposted with permission from The Conversation.

 233k
233k  41k
41k  Subscribe
Subscribe 